 |
|
|
 |
| Current Status and Future for Pulmonary
Embolism |
|
Yasuhiro Satoh, M.D.
Shakai-Hoken Mishima Hospital,
Japan
Norikazu Yamada, M.D.
Mie University, Tsu, Japan
Russell D. Hull, M.D.
University of Calgary, Calgary,
Canada |
|
|
|
 |
|
|
 |
|
| In Japan, the incidence
of pulmonary thromboembolism (PTE) is increasing. This
seems to be related to a more Westernized lifestyle
and an older population whose risk for venous thromboembolism
is increased due to inactivity and the high prevalence
of conditions such as stroke, ischemic heart disease,
heart failure and cancer. Three therapeutic approaches
to PTE reviewed in this session are anticoagulation
therapy, thrombolytic therapy and inferior vena cava
(IVC) filter. |
|
Outcomes
with Inferior Vena Cava Filter |
The mortality associated
with pulmonary embolism (PE) has increased 3-fold in
the last 10 years. The diagnosis and treatment of acute
PE in Japan is lacking, as shown by the differences
in incidence and mortality between hospitals. At the
Shakai-Hoken Mishima Hospital in Japan, the placement
of temporary IVC filters (T-IVCF), unless contraindicated,
to prevent acute recurrence of PE has been part of the
established therapeutic protocol since 1996. The indications
for a T-IVCF for primary prevention are for high-risk
patients undergoing gynecological or orthopedic surgery
with leg edema and/or high serum D-dimer and with thrombolytic
therapy for deep vein thrombosis.
Thrombolytic therapy with the protection of a T-IVCF
for acute PE decreased the recurrence of PE and shortened
hospitalization, concluded Yasuhiro Satoh, MD, in reviewing
data from their retrospective study of the experience
at Shakai-Hoken Mishima Hospital. Of 44 consecutive
PE patients who had received conventional therapy of
heparin and thrombolytic therapy, 10 received a T-IVCF
only and 26 received only conventional therapy (the
others had a permanent IVCF). In-hospital recurrence
of PE was seen in 1 of the 10 (10%) T-IVCF patients,
compared to 10 of the 26 (38%) conventional therapy
patients. Placement of a permanent IVCF was required
in 4 of the 26 conventional therapy patients due to
secondary PE, compared to none in the T-IVCF group.
A shorter hospital stay was found in the T-IVCF group
(20.3 days) compared to the conventional therapy group
(31.9 days) and permanent IVCF group (55 days). No PE
recurrence was reported during the mean 33 months follow-up.
In the T-IVCF group, there was 1 death due to cerebellar
hemorrhage, while other major complications were comparable.
|
PAGE
TOP
|
Outcomes
with Conventional Therapy in Japan |
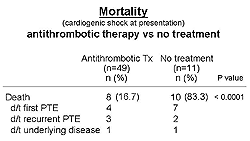 |
| Figure
1. Mortality rates and etiology in 60 patients
with acute pulmonary thromboembolism. |
| Click
to enlarge |
|
Antithrombotic
therapy and prevention of recurrence seems to improve
the clinical outcome of acute PTE. However, a favorable
effect for thrombolysis in terms of outcomes was not
demonstrated in Japanese patients with acute PTE, as
reported in Western countries, stated Norikazu Yamada,
MD, of Mie University, based on data from three analyses.
These analyses were of patients in shock or clinically
stable at presentation to Mie University Hospital, and
a registry cohort. Yamada stated that limitations of
the retrospective analyses include the selection bias
that thrombolytic therapy may be more frequently used
than heparin in severe acute PTE, and that the association
between right ventricular function and the clinical
outcome was not evaluated. Large prospective trials
comparing thrombolytic therapy and heparin are required
in Japan.
In 60 patients with acute PTE presenting in cardiogenic
shock (systolic blood pressure < 90 mm Hg for >
15 min), the in-hospital mortality was significantly
improved in the 49 patients with antithrombotic therapy
compared to the 11 patients with no therapy (Figure
1). Age > 65 years (odds ratio 8.44; p=0.03) was
shown to be a significant predictor of in-hospital mortality
by logistic regression analysis. The evaluation of deep
vein thrombosis (DVT) was a predictor of in-hospital
mortality in the antithrombotic therapy patients (odds
ratio 0.014; p=0.012). |
 |
| Figure
2. Clinical events in patients who were clinically
stable at the initiation of treatment based on
treatment and no treatment. |
| Click
to enlarge |
|
No significant
difference in in-hospital mortality between thrombolysis-treated
or anticoagulation-treated patients were observed amongst
97 patients with acute PTE who were hemodynamically
stable at the initiation of treatment, regardless of
presence of cardiogenic shock at presentation (Figure
2). Nineteen patients received no antithrombotic therapy.
There was no significant difference in clinical events
in hospital in relation to thrombolytic therapy (n=53;
2 deaths) or heparin therapy (n=25, 1 death). Recurrent
PTE was the cause of death in both treatment groups
and the incidence of major bleeding was similar. Age
> 65 years (odds ratio 47.91; p=0.043) and cardiogenic
shock (odds ratio 52.72; p= 0.043) were predictors of
in-hospital mortality. |
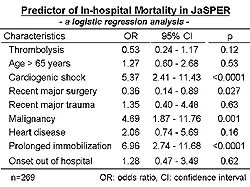 |
| Figure
3. Predictors of In-hospital mortality in patients
with acute pulmonary thromboembolism in the Japanese
Society of Pulmonary Embolism Research registry. |
| Click
to enlarge |
|
The effect of
thrombolytic versus anticoagulation therapy on in-hospital
mortality was retrospectively evaluated in patients
with acute PTE registered in the Japanese Society of
Pulmonary Embolism Research (JaSPER) registry. Acute
PTE was managed with thrombolysis in 155 patients (urokinase
110 patients, tPA 58 patients) and anticoagulation therapy
only in 114 patients. No significant difference was
seen in total mortality between the groups (20 versus
5 deaths, respectively). In patients with cardiogenic
shock, thrombolysis was used in 73 patients and anticoagulation
only in 18 patients. No between group difference in
mortality was seen (15 versus 2 deaths, respectively).
The predictors of mortality on logistic regression analysis
were cardiogenic shock, malignancy, and prolonged immobilization
(Figure 3). |
PAGE
TOP
|
PE Therapy
with Low Molecular Weight Heparin |
Low molecular weight heparin
(LMWH) represents a therapeutic advance, and will simplify
the treatment of PE and DVT in Japan, stated Russell
D. Hull, MD, of the University of Calgary in Canada.
The approach to diagnosis and treatment of PE and DVT
are similar regardless of patient presentation (lung,
legs). The underlying precursor and proximal vein thrombosis
in particular must also be considered.
LMWH offers many benefits, such as convenient outpatient
treatment, lower cost since monitoring is not needed
and earlier hospital discharge for home-based treatment.
LMWH treatment may result in slightly less recurrent
VTE and may offer a survival benefit in patients with
cancer. Intravenous therapy for PE or DVT is not required
with LMWH due to its high bioavailability (90% with
subcutaneous administration, compared to 30% bioavailability
for unfractionated heparin). The long half-half of LMWH
provides for administration only 1-2 times per day.
In Canada and the US, once daily subcutaneous injections
is standard therapy. The anticoagulant response is highly
correlated with body weight, thus monitoring of the
anticoagulant response is not needed, as it is with
unfractionated heparin (UH).
In an equivalency trial Hull and colleagues showed that
the once daily subcutaneous LMWH tinzaparin was as effective
as intravenous heparin, with a trend towards superiority
with a risk reduction of 58%, in the setting of proximal
DVT. Tinzaparin was safer than heparin, with a 91% risk
reduction in major bleeding (p=0.006). The overall bleeding
rate for major bleeding was 5% in the heparin group
and 0.5% in the LWMH group. Surprisingly, there was
a 51% risk reduction in mortality, from 21 deaths in
the heparin group to 10 deaths in the LMWH group.
Enoxaparin has been shown to have a risk reduction of
22% for recurrent VTE and 34% risk reduction for death.
In a study of 612 patients with PE by Simonneau and
colleagues, the LMWH tinzaparin was shown to be equivalent
to UH in terms of death, recurrent VTE, major bleeding,
and occurrence of at least 1 outcome event. This finding
was supported by a study by Hull and colleagues. In
this study, in 200 patients with VTE, tinzaparin plus
warfarin was associated with a treatment duration of
6 days and no objectively diagnosed recurrent VTE or
fatal PE, while intravenous heparin plus warfarin was
associated with a treatment duration of 6 days, 7 objectively
diagnosed recurrent VTE (p=0.009) and 1 death.
The superiority of LMWH seen in the Hull trial, but
not seen in the Simonneau trial, is due to a higher
rate of previous surgery (54.5% vs 15.6%, respectively),
higher rate of cancer (31% vs 9.8%), lower rate of previous
VTE (17.5% vs 27.1%) and lower rate of heart disease
(15.5% vs 22%). Further, all of the patients in the
Hull study and only 50% of the patients in the Simonneau
study had proximal venous thrombosis. Thus, proximal
venous thrombosis plus PE is a more serious disorder
than PE alone.
The evolution of the more routine use of LMWH and 2-D
echocardiography to visualize clot burden may allow
for more effective use of thrombolysis for PE. Right
ventricular (RV) dysfunction is associated with a mortality
rate of 16-22% over 20-90 days. Hull suggests that the
use of 2D echo may be useful for patient selection when
considering thrombolysis. RV wall motion has been shown
to improve in patients treated with tPa compared to
heparin alone (39% vs 17% improved, respectively), and
this improvement is correlated with a lower recurrence
rate in the tPA group. However, the trial was small
and further studies are needed to establish a standard
of care in terms of thrombolysis.
The use of thrombolytic therapy in the treatment of
DVT and PE remains highly individualized. In general,
patients with hemodynamically unstable PE or massive
ilio femoral thrombosis, with a low bleeding risk, are
the most appropriate candidates. Early use of thrombolytic
agents decreases subsequent pain, swelling and loss
of valves. Some studies have shown a decrease in the
incidence of post-phlebotic syndrome associated with
the use of thrombolytic agents. In patients with DVT,
urokinase and streptokinase are approved for 48 to 72
hours of therapy. Patients who receive thrombolytic
therapy have a 1-2% risk of intracranial bleeding. |
PAGE
TOP
|
Report
Index | Previous Report
| Next Report
Scientific
Sessions | Activities
| Publications
Index
Copyright © 2001
Japanese Circulation Society
All Rights Reserved.
webmaster@j-circ.or.jp
|
|